Technology Conference Listing
Featured: Women in STEM Conference and Award, San Francisco, Sept 10-12, 2017
Featured: PrecisionAg Vision Conference, Phoenix, Oct 10-12, 2017
Featured: SPTechCon, SharePoint Technology Conference, Washington, DC, Nov 12-15, 2017
San Francisco Professional Events List
 Please wait...
Please wait...
Advanced Specialty Coding, Compliance & Reimbursement Symposium (BLR)
Date
Link to Website
Organizer
Venue
Location
Advanced Specialty Coding, Compliance & Reimbursement Symposium 2020
Prepare for 2020 with a first look at coding, payment and policy changes that will impact your specialty practice
Sharpen your coding and billing skills, clean up documentation, minimize audit risk, and ensure that your practice optimizes revenue with the tools, tips and guidance you’ll get from our expert panel of speakers at this year’s Advanced Specialty Coding, Compliance & Reimbursement Symposium.
Join us for this must-attend event to get the specialty-specific training you need to code appropriately. Plus, get a first look at the new procedure codes you'll use in 2020 and the diagnosis codes that went into effect on Oct. 1 so you can be certain you're correctly reporting both code sets. We’ll cover all the hot topics and answer your most pressing questions.
Select from four specialty tracks – Anesthesia, Orthopedics, Pain Management,Hierarchical Condition Categories – and take a deep dive in to your specialty.
-
Hierarchical Condition Categories – Healthcare providers face a 5% pay cut to all Medicare reimbursement based on their 2020 reporting – find out how to avoid greater pay cuts in the near future
-
Take a first look at 2020 CPT® codes – get a glimpse from experts in the field on how these changes are likely to impact practices
-
Get the latest ICD-10-CM updates – make sure you understand the new codes and guidelines
-
Prepare for clinical documentation integrity – find out what you need to know as a coder to help your clinicians document in accordance with quality measures
-
Learn to succeed at new coding challenges – including risk adjustment coding and Medicare’s merit-based incentive payment system (MIPS)
-
Ask the Expert – get your specialty-specific questions answered by our coding experts during every session and an open Q&A
-
Select different specialty tracks for preconference and main conference – multi-specialty practices can get the training needed at one conference
ANESTHESIA
Get answers to your questions about the new anesthesia for GI endoscopy codes; protect your practice with a compliance program that is custom-made for your practice; learn the latest about requirements for post-op pain procedures. These are just three of the information-packed sessions designed to show anesthesia practices how to overcome their toughest billing, coding and compliance challenges.
ORTHOPEDICS
Join the nation’s top orthopedic coding experts as they provide you with the most comprehensive, accurate surgical and ICD-10-CM coding guidance, as well as tested strategies to ensure you meet payers’ latest documentation requirements.
PAIN MANAGEMENT
Learn how to boost revenue with smart selection of ancillary services; improve your comorbidity coding to meet medical necessity requirements and support E/M visits, and make sure E/M visits during the global period will stand up the latest RAC audit. Want more? There’s plenty more. This year’s pain management conference will teach pain management practices how to take their billing, coding and compliance to a higher level.
HIERARCHICAL CONDITION CATEGORIES
Hierarchical Condition Categories are here to stay and we’ve added a track dedicated to this single issue. Join our experts as they teach participants how to apply new coding methodologies to boost your bottom line.
Expert Speakers

Judith Blaszczyk RN, CPC, ACS-PM | Medical Compliance Auditor, Auditing for Compliance and Education, Inc.
Judith Blaszczyk has 19 years of experience as a registered nurse working in an acute care hospital setting. This background provides invaluable insight into the clinical aspects of medical coding and documentation as well as experience interacting with physicians and other clinicians. In addition to her clinical background, Blaszczyk has more than 28 years of experience in medical coding and billing, specializing in anesthesia and pain management.

Doris Branker CPC, CPC-I, CPMA, CIRCC, CANPC, CEMC | President, DB Healthcare Consulting
Doris Branker has a practice management consulting firm that also offers medical coding preparation camps. Dori is a nationally-recognized educator, coding expert, and practice management consultant, as well as an approved educator and PMCC licensed instructor with AAPC. Her areas of expertise include medical coding, compliance, auditing, billing and collections management. She holds specialty certifications in E/M, Interventional Radiology, and Cardiovascular coding.

Kelly Dennis MBA, ACS-AN, CANPC, CHCA, CPC, CPC-I | President, Perfect Office Solutions
Kelly Dennis has more than 35 years of experience in physician billing and office administration. She is a certified coder with AAPC; a PMCC certified instructor; and received a Certificate of Proficiency in Anesthesiology from AAPC in 2001. She is also an Advanced Coding Specialist in Anesthesia and has served as lead anesthesia advisor for the Board of Medical Specialty Coding since 2004.

Brenda Edwards CPC, CDEO, CPB, CPMA, CPC-I, CEMC, CRC, AAPC Fellow |
Brenda has been involved in the healthcare arena for over 25 years with experience in chart audit, coding and billing, education, consulting, practice management and compliance. She has worked closely with practices, providers and residency programs to ensure documentation is compliant and accurate. Brenda has written many articles for national publications including Healthcare Business Monthly, American Academy of Family Physicians (AAFP) and BC Advantage. Her humorous and engaging presentation style has made her a conference favorite at both national and regional conferences for AAPC as well as local chapter meetings across the country. Brenda is also an AAPC workshop and webinar presenter. Brenda has assisted countless students obtain their coding credentials through the AAPC Professional Medical Coding Curriculum. She is also an AAPC ICD10-CM/PCS Training Expert. She served on the AAPC Chapter Association Board of Directors from 2010-2020 and held office as Chair. She has been intimately involved in the development and continuation of the Hardship Scholarship Program for AAPC. Mentoring fellow members of AAPC is a passion for her. She is co-founder of the northeast Kansas (NEKAAPC) AAPC chapter and has served many offices.

Annmarie A. Edwards DPM, FACFAS, FACFAOM |
Dr. Edwards has been with Intermountain Healthcare for the past 14 years. She is not only dedicated to providing the best foot and ankle care possible for her patients but is also involved with resident training. Her educational background includes graduating from Temple University School of Podiatric Medicine with her residency at the Veterans Administration Medical Center, Salt Lake City, Utah. She has been recognized as a national speaker, has served on many national committees representing not only podiatric medicine but also an advocate for residency training. Dr. Edwards has a special interest in the treatment of the various medical issues with the diabetic foot. She also established a non-profit organization with other physicians that travels to Tonga to perform limb salvage operations and do educational services to decrease the amount of amputations in Tonga.

Scott R. Grubman
Scott R. Grubman is a partner with the law firm of Chilivis Cochran in Atlanta, Georgia. He focuses his practice on representing healthcare providers of all types and sizes in connection with government investigations and compliance-related matters. Prior to joining private practice, Grubman served as both a trial attorney for the United States Department of Justice in Washington, D.C., and as an Assistant United States Attorney in Savannah, Georgie where he served on his district’s healthcare fraud task force and was responsible for investigating and litigating healthcare fraud matters on behalf of the United States.

Kayla Lee
Kayla Lee, CPC joined the Auditing for Compliance and Education, Inc. (ACE) team in November 2020. Ms. Lee has spent the past several years under the mentorship of ACE’s president and nationally known expert in anesthesia and pain management Devona Slater, CHC, CHA, CMCP. Kayla holds a Certified Professional Coding (CPC) certification. While working at ACE she has been instrumental in cultivating the ACE coding division that provides a coding service, producing over 80,000 cases a month for groups across the country. Prior to that, she worked as a Certified Pharmacy Technician after graduating from Kansas State University. Kayla is very passionate about the anesthesia industry and believes that education for coders and providers is instrumental in creating the best coding service.

Erica Remer MD, FACEP, CCDS |
Erica Remer has a unique perspective as a practicing emergency physician for 25 years, with extensive coding, CDI, and ICD-10 expertise. As Physician Advisor of a large multi-hospital system for four years, she trained 2700 providers in ICD-10, closed hundreds of queries, and fought numerous DRG clinical validation and medical necessity denials. Dr. Remer transitioned to independent consulting in July 2020 and has since authored numerous articles on CDI topics. Her real passion is educating coders, CDI specialists, and healthcare providers. You may know her from being the co-host of Talk Ten Tuesdays, a weekly national podcast. For fun, she participates in ICD-10 Coordination and Maintenance Committee meetings.

Devona Slater CHA, CMCP, CHC | President, Auditing for Compliance and Education, Inc.
Devona Slater is a strong ally to both physicians and their patients. For more than a decade, she has been committed to helping physicians manage their practices so they can devote more time to doing what they were trained to do – practice medicine. Slater has served as president and compliance auditor specializing in anesthesia and pain management issues for the past 17 years. She has helped numerous anesthesia and pain management professionals across the nation with billing, coding and compliance issues.

Stephanie Thomas CANPC, CPC | Billing Director, CE Medical Group
Stephanie has been in the medical field for 18 years. Thomas has experience in multiple specialties of medical billing and coding, and is a certified pain and anesthesia coder. Billing is her passion, which is why she’s efficient at maximizing reimbursements while educating providers and staff on proper coding techniques. She motivates and coaches her billers to ensure they achieve a high level of standards. Thomas enjoys speaking at national conferences and sharing her knowledge in the pain medicine billing and practice management realm.

Amy Turner RN, BSN, MMHC, CPC | Director of Billing Compliance for CE Medical Group
Amy Turner has been in the healthcare field since 1989 when she completed her Associates Degree in Nursing at Middle Tennessee State University. Amy then continued her education at MTSU by receiving her Bachelors of Science in nursing, follow by a MMHC from Vanderbilt University’s Owen Graduate School of Management. She began her nursing career as a charge nurse of the ICU at Middle Tennessee Medical Center in Murfreesboro, Tennessee. Ten years after beginning her career in healthcare, Amy focused her career in Pain Management. She is currently the Director of Billing Compliance for CE Medical Group.

Margie Scalley Vaught CPC, CPC-H, CCS-P, MCS-P, ACS-EM, ACS-OR | Margie Scalley Vaught and Associates
With 20+ years focused exclusively in orthopedics, Margie has a unique ability to translate coding, billing and reimbursement rules into real-world practice, (95% of attendees from previous conferences rate Margie a 10 out of 10 speaker!) She is technical editor to DecisionHealth’s Orthopedic Coder’s Pink Sheet and author of orthopedic specialty guides. She conducts day-to-day procedure coding and deciphers operative reports for orthopedic practices nationwide.
Agenda
*Agenda Subject to Change
Select from four specialty-specific tracks. You may register for a different preconference specialty track from a main conference specialty track
ANESTHESIA
PRECONFERENCE
Monday, October 15
8:00 a.m. – 9:00 a.m.
Registration, Continental Breakfast
9:00 a.m. – 10:15 a.m.
Risk reduction plan: a compliance workshop for anesthesia practices
Devona Slater
Knowledge is power and protection. Prosecutors have learned that improper billing and coding make physician practices easy targets. In the past year dozens of practices have had to write checks for hundreds of thousands, even millions of dollars, to settle allegations of fraud. The only way an anesthesia practice can protect itself is with a knowledge-driven compliance program. This session will show you how to keep up with the latest billing and coding rules; ways to effectively educate clinical and administrative staff; best practices for regular internal reviews and audit response and what to do when someone on the staff comes forward with compliance concerns.
10:15 a.m. – 10:45 a.m.
Morning Break
10:45 a.m. – 12:00 p.m.
The new quality performance landscape for anesthesia – lessons learned in the first two years of MIPS
Kelly Dennis
CMS and Congress have made tweaks to the merit-based incentive payment system but the program isn’t going away. Get caught up on MIPS and prepare for Year 3 with this specialty-specific session. Review lessons learned from the first two years of the program; find how the return of the cost category could impact your practice; get the facts on patient facing and non-patient facing clinicians; find out how the Bipartisan Budget Act of 2020 will impact the program in coming years and get an idea of what to expect in 2020 based on the proposed rule.
Bonus: This session will introduce you to the five new patient relationship modifiers which will be used to calculate cost in coming years.
12:00 p.m. – 1:00 p.m.
Networking Lunch
1:00 p.m. – 2:15 p.m.
Collections for anesthesia services
Devona Slater
Believe it or not: Collecting payments from patients doesn’t have to be an agonizing process for patients and practice members. When patients don’t pay, a practice that doesn’t have an effective collections program could lose revenue, alienate patients, and break the law. Stop sweating collections. This session, which is designed exclusively for the challenges anesthesia practices faces, show you how to create a “collections culture” at your practice that makes capturing payment at the earliest possible stage and effective follow up for uncollected payment automatic.
2:15 p.m. – 3:30 p.m.
“ANESTHESIA CARE NOT TYPICALLY REQUIRED.” Now what?
Kelly Dennis
The 2020 ASA crosswalk changed the status of 26 procedures to -00004: anesthesia care not typically required, including more than a dozen interventional pain management procedures. During this session you’ll learn the ASA’s reasoning on -00004 status procedures, get guidance for reporting other forms of sedation such as moderate sedation and find out how to appeal a denial when you feel anesthesia was required for a specific case.
3:30 p.m. – 4:00 p.m.
Afternoon Break
4:00 p.m. – 5:15 p.m.
Opioid prescriptions – Don’t panic, get the facts
Scott Grubman
Opioid abuse has been in the headlines and on the minds of policy makers and law makers. Providers are being drafted to help fight opioid abuse, threatened with penalties if they don’t comply with stringent laws, and they still need to take care of their patients. Don’t let misinformation lead to mistakes. Come to this session for accurate information about the government’s new enforcement initiatives related to opioids. You’ll leave with the facts about what prescribers are required to do, and how to protect the practice from penalties.
(This session will include Orthopedic and Pain Management attendees.)
MAIN CONFERENCE DAY 1
Tuesday, October 16
7:00 a.m. – 8:00 a.m.
Registration, Continental Breakfast with Exhibitors
8:00 a.m. – 9:00 a.m.
Keynote Presentation
The doctor is in: A clinician shares her top ICD-10-CM cures for common coding disorders
Erica E. Remer, MD, FACEP, CCDS, Founder and President, Erica Remer, MD, Inc. Consulting Services in Clinical Documentation, CDI, and ICD-10
Hierarchical conditions and quality-based revenue demand more accurate and complete diagnosis coding, supported by physician documentation. In this down-to-earth session, medical doctor and clinical documentation improvement expert Erica Remer, MD shares examples of commonly misunderstood ICD-10-CM guidelines and conditions. She’ll clear up your confusion and give you pointers to help your providers. Along the way, you’ll learn the most efficient ways to query physicians to get the full diagnostic picture of the patient’s condition and optimize your practice’s documentation, coding and reimbursement.
9:00 a.m. – 9:15 a.m.
Early Morning Break
9:15 a.m. – 10:30 a.m.
Anatomy for anesthesia coding and billing staff
Doris Branker
Improve your knowledge of anatomy, your understanding of anesthesia charts and your ability to spot documentation gaps. Attend this session that mirrors the pre-operative exams your clinicians perform every day, including the oral cavity; the pulmonary system, the cardiovascular system and the nervous system.
10:30 a.m. – 11:00 a.m.
Midmorning Break with Exhibitors
11:00 a.m. – 12:15 p.m.
Coding the comorbidities and conditions that impact anesthesia care
Kayla Lee
A patient’s condition does more than shape the anesthesia provider’s plan of care, it can determine whether a payer will cover anesthesia services at all. During this session you’ll get the latest guidance on coding conditions that impact anesthesia care such as:
- Hypertension
- Diabetes
- COPD
- Movement disorders
And because you can’t code it if it isn’t documented, you’ll get tips for educating clinical staff about how to capture the information you need to support your diagnosis coding.
12:15 p.m. – 1:15 p.m.
Networking Lunch with Exhibitors
1:15 p.m. – 2:30 p.m.
Arthroplasty: Don’t let your anesthesia claims get out of joint
Stephanie Thomas
Anesthesia services for joint replacement services such as total knee arthroscopy may involve regional or general anesthesia. During this session you’ll learn the latest about the documentation and coding requirements for the pain management techniques anesthesia clinicians are using today.
2:30 p.m. – 3:00 p.m.
Afternoon Break with Exhibitors
3:00 p.m. – 4:15 p.m.
Teach your anesthesia staff how to write their lines, and learn about new codes
Judi Blaszcyk
At the end of this session you’ll be ready to train anesthesia providers to quickly create complete documentation for all of their lines including:
- Arterials
- PICC
- Swan-Ganz
You’ll have answers to such questions as whether you need to document pressure to report Swan-Ganz and how important vessel patency is to reporting ultrasound guidance services. You’ll also know about the new and revised PICC line codes that will go into effect next year.
4:15 p.m. – 5:30 p.m.
Endoscopy FAQ: Answers to the top 10 GI endoscopy questions
Devona Slater
Confusing guidance from Medicare and private payers, modifier use and reporting combined upper and lower GI endoscopy services are just three challenges anesthesia practices faced thanks to this year’s new anesthesia codes. This session will provide solutions to the documentation, coding and billing problems that plagued practices across the nation.
MAIN CONFERENCE DAY 2
Wednesday, October 17
7:00 a.m. – 8:00 a.m.
Continental Breakfast with Exhibitors
8:00 a.m. – 9:15 a.m.
POP, PCA and pain rounds
Kelly Dennis
Make sure your practice is up-to-date on the requirements for post-operative pain management to Medicare and private payers. Learn the three elements the anesthesia provider must capture in the note; how to report patient-controlled anesthesia and get tips for documenting and reporting pain rounds.
9:15 a.m. – 10:30 a.m.
Overcome current medical direction documentation challenges
Devona Slater
Medical direction is still on the HHS Office of Inspector General’s radar, and anesthesiologists still struggle to produce documentation that will protect them and the practice from improper payments and punitive fines. Find out what one veteran consultant sees when she reviews medical direction documentation and get expert tips for making sure your claims will withstand review.
10:30 a.m. – 11:00 a.m.
Morning Break with Exhibitors
11:00 a.m. – 12:15 p.m.
Nobody’s perfect – learn the mistakes made by the best coders and billers, and stop making them
Judi Blaszczyk, Doris Branker, Devona Slater, Stephanie Thomas
Our expert speakers see it all, as they help anesthesia and pain management practices around the country. They even see the mistakes made by billers and coders with years of experience. Come to this combined session to learn about the errors even experienced claims staff make and find out how to eliminate the mistakes from your practice.
12:15 p.m. – 12:45 p.m.
Ask the experts – Open Q&A
12:45 p.m.
Conference Adjourns
ORTHOPEDICS
PRECONFERENCE
Monday, October 15
8:00 a.m. – 9:00 a.m.
Registration, Continental Breakfast
9:00 a.m. – 10:15 a.m.
Reduce fracture coding headaches and ensure proper reimbursement
Margie Scalley Vaught
Review documentation, procedure and ICD-10-CM coding requirements for fractures, as well as potential compliance risk areas to avoid for these services. You’ll learn the key points that must be documented to select the most specific fracture diagnosis code, when and how to report fixation, debridement and casting, and the best ways to manage tricky global period scenarios involving multiple care providers.
10:15 a.m. – 10:45 a.m.
Morning Break
10:45 a.m. – 12:00 p.m.
Correctly code orthopedic injections
Margie Scalley Vaught
With payers increasing their scrutiny of orthopedic injection claims, it’s more important than ever for practices to stay up to date on documentation, coding and billing rules to avoid audits and denials. In this session, you’ll get the most current guidance for your top injection procedures including viscosupplementation, Dupuytrens, tendon sheath injections and trigger points. Properly report imaging including ultrasound when medically necessary and quickly determine when a separate E/M code can be billed.
12:00 p.m. – 1:00 p.m.
Networking Lunch
1:00 p.m. – 3:30 p.m.
Shore up your spine coding
Margie Scalley Vaught
If you’ve noticed reimbursement dwindling for spine surgeries in recent months, you’re not alone. Payers are tightening up coding and billing requirements for fusions, corpectomies, grafts and instrumentation with new code bundling and documentation policies. To ensure appropriate payment, get detailed examples of how to meet CPT® and payer requirements for plates and cages, laminotomies and other critical spine procedures.
3:30 p.m. – 4:00 p.m.
Afternoon Break
4:00 p.m. – 5:15 p.m.
Opioid prescriptions – Don’t panic, get the facts
Scott Grubman
Opioid abuse has been in the headlines and on the minds of policy makers and law makers. Providers are being drafted to help fight opioid abuse, threatened with penalties if they don’t comply with stringent laws, and they still need to take care of their patients. Don’t let misinformation lead to mistakes. Come to this session for accurate information about the government’s new enforcement initiatives related to opioids. You’ll leave with the facts about what prescribers are required to do, and how to protect the practice from penalties.
(Combined session with Anesthesia, Pain Management tracks)
MAIN CONFERENCE DAY 1
Tuesday, October 16
7:00 a.m. – 8:00 a.m.
Registration, Continental Breakfast with Exhibitors
8:00 a.m. – 9:00 a.m.
Keynote Presentation
The doctor is in: A clinician shares her top ICD-10-CM cures for common coding disorders
Erica E. Remer, MD, FACEP, CCDS, Founder and President, Erica Remer, MD, Inc. Consulting Services in Clinical Documentation, CDI, and ICD-10
Hierarchical conditions and quality-based revenue demand more accurate and complete diagnosis coding, supported by physician documentation. In this down-to-earth session, medical doctor and clinical documentation improvement expert Erica Remer, MD shares examples of commonly misunderstood ICD-10-CM guidelines and conditions. She’ll clear up your confusion and give you pointers to help your providers. Along the way, you’ll learn the most efficient ways to query physicians to get the full diagnostic picture of the patient’s condition and optimize your practice’s documentation, coding and reimbursement.
9:00 a.m. – 9:15 a.m.
Early Morning Break
9:15 a.m. – 10:30 a.m.
Shake up your pelvis and hip coding
Margie Scalley Vaught
Refresh your understanding of the coding for key hip and pelvis procedures including fracture treatment, hip replacement, femoral acetabular impingement surgery, as well as the appropriate ICD-10-CM codes and documentation requirements that support them. Also learn coding of total hip revision, fasciotomy and treatment of hip dysplasia, slipped epiphysis and hip core decompression
10:30 a.m. – 11:00 a.m.
Midmorning Break with Exhibitors
11:00 a.m. – 12:15 p.m.
Bolster your knee coding
Margie Scalley Vaught
Ensure you are current with coding, documentation and payer policy changes for your top knee procedures, including arthroscopy, joint replacement, ligament repair, OATS procedures, subchondroplasty and more. Get accurate, up-to-date information about the most recent payer policies – including the National Correct Coding Initiative – for both open and arthroscopic procedures.
12:15 p.m. – 1:15 p.m.
Networking Lunch with Exhibitors
1:15 p.m. – 2:30 p.m.
Repair shoulder coding to ensure proper reimbursement
Margie Scalley Vaught
Learn the difference between a shoulder repair and a reconstruction, a tenotomy and a tenolysis. Find out how to tell a SLAP lesion repair from a capsulorrhaphy and when a coracoacromial ligament release should be reported instead of a partial acromionectomy. Find out the most appropriate way to code an open repair with an arthroscopic acromioplasty. And stay current on NCCI coding policy for shoulder arthroscopy to reduce audit and denial risk.
2:30 p.m. – 3:00 p.m.
Afternoon Break with Exhibitors
3:00 p.m. – 4:15 p.m.
Repair should coding to ensure proper reimbursement (continued)
4:15 p.m. – 5:30 p.m.
Strengthen Elbow and forearm repair coding
Margie Scalley Vaught
Learn how to code fasciotomy of the upper extremity and the components of an olecranon bursectomy – and what may be reported separately. Resolve confusion around tendon reinsertion and repair, and identifying collateral ligaments from a coding perspective. Make sure you are properly reporting nerve repair services such as cubital tunnel release.
MAIN CONFERENCE DAY 2
Wednesday, October 17
7:00 a.m. – 8:00 a.m.
Continental Breakfast with Exhibitors
8:00 a.m. – 10:30 a.m.
Tighten your grip on hand, finger and wrist coding
Margie Scalley Vaught
Address coding of wrist procedures including fracture and dislocation repair, wrist scopes and basal joint arthroplasty as well as carpal tunnel procedures, nerve wraps and re-dos. See how the new nerve allograft codes fit into repair procedures as you clear up your understanding of hand and finger tendon, nerve and artery repairs, including those that occur in Zone 2, as well as chronic injuries such as trigger finger and gamekeeper’s thumb.
10:30 a.m. – 11:00 a.m.
Morning Break with Exhibitors
11:00 a.m. – 12:45 p.m.
Get a clinician’s view of coding key foot and ankle procedures
Annmarie A. Edwards
In this session, you’ll gain an understanding of the different types of bunion repairs, as well as toe, foot and ankle fracture reductions, and the services involved in limb salvage, such as debridement. In addition, get a glimpse of the changing ICD-10-CM coding challenges doctors are facing for these services.
12:45 p.m.
Conference Adjourns
PAIN MANAGEMENT
PRECONFERENCE
Monday, October 15
8:00 a.m. – 9:00 a.m.
Registration, Continental Breakfast
9:00 a.m. – 10:15 a.m.
Risk reduction plan: A compliance workshop for pain management practices
Amy Turner
Does your practice have $2 million to spare? If not, it needs to make sure it has an air-tight compliance program. Last year a pain management practice in New York was just one of many medical practices that learned the hard – and expensive way – that prosecutors are pursing practices that improperly bill and code services and winning multi-million dollar settlements. This session will show you how to keep up with the latest billing and coding rules; ways to effectively educate clinical and administrative staff; best practices for regular internal reviews and audit response and what to do when someone on the staff comes forward with compliance concerns.
10:15 a.m. - 10:45 a.m.
Morning Break
10:45 a.m. – 12:00 p.m.
The new quality performance landscape for pain management – lessons learned in the first two years of MIPS
Stephanie Thomas
CMS and Congress have made tweaks to the merit-based incentive payment system but the program isn’t going away. Get caught up on MIPS and prepare for Year 3 with this specialty-specific session. Review lessons learned from the first two years of the program; learn how the return of the cost category could impact your practice; get the facts on patient facing and non-patient facing clinicians; find out how the Bipartisan Budget Act of 2020 will impact the program in coming years and get an idea of what to expect in 2020 based on the proposed rule.
Bonus: This session will introduce you to the five new patient relationship modifiers which will be used to calculate cost in coming years.
12:00 p.m. – 1:00 p.m.
Networking Lunch
1:00 p.m. – 2:15 p.m.
Collections for pain management practices
Doris Branker
Patient payments. They’re vital to the practice and not collecting them can constitute fraud. When patients don’t pay, a practice that doesn’t have an effective collections program could lose revenue, alienate patients, and break the law. Stop sweating collections. At the end of this specialty-specific session you’ll be ready to create a “collections culture” at your practice that makes capturing payment at the earliest possible stage and ensures that effective follow up for uncollected payment is automatic.
2:15 p.m. – 3:30 p.m.
Adding ancillary services to the pain management practice, the right way, the smart way, the easy way
Stephanie Thomas
Ancillary services can improve patient care and bring a much-needed revenue boost to the practice. They also can leave a practice holding expensive equipment that will never bring in the revenue promised by a vendor. Learn how to add ancillary services the right way. At the end of this session you’ll know how to:
-
Fact-check the vendor’s sales pitch
-
Select services that make sense for your practice
-
Gauge the cost
-
Estimate revenue
-
Educate staff
-
Avoid common pitfalls
3:30 p.m. – 4:00 p.m.
Afternoon Break
4:00 p.m. – 5:15 p.m.
Opioid prescriptions – Don’t panic, get the facts
Scott Grubman
Opioid abuse has been in the headlines and on the minds of policy makers and law makers. Providers are being drafted to help fight opioid abuse, threatened with penalties if they don’t comply with stringent laws, and they still need to take care of their patients. Don’t let misinformation lead to mistakes. Come to this session for accurate information about the government’s new enforcement initiatives related to opioids. You’ll leave with the facts about what prescribers are required to do, and how to protect the practice from penalties.
(This session will include Anesthesia and Orthopedic attendees.)
MAIN CONFERENCE DAY 1
Tuesday, October 16
7:00 a.m. – 8:00 a.m.
Registration, Continental Breakfast with Exhibitors
8:00 a.m. – 9:00 a.m.
Keynote Presentation
The doctor is in: A clinician shares her top ICD-10-CM cures for common coding disorders
Erica E. Remer, MD, FACEP, CCDS, Founder and President, Erica Remer, MD, Inc. Consulting Services in Clinical Documentation, CDI, and ICD-10
Hierarchical conditions and quality-based revenue demand more accurate and complete diagnosis coding, supported by physician documentation. In this down-to-earth session, medical doctor and clinical documentation improvement expert Erica Remer, MD shares examples of commonly misunderstood ICD-10-CM guidelines and conditions. She’ll clear up your confusion and give you pointers to help your providers. Along the way, you’ll learn the most efficient ways to query physicians to get the full diagnostic picture of the patient’s condition and optimize your practice’s documentation, coding and reimbursement.
9:00 a.m. – 9:15 a.m.
Early Morning Break
9:15 a.m. – 10:30 a.m.
Anatomy for pain management coding and billing staff
Amy Turner
Improve your knowledge of anatomy, your understanding of procedure notes and your ability to spot documentation gaps. Attend this session that focuses on the body systems your providers treat every day:
-
Muscles and tendons
-
Bones and joints
-
Nerves
10:30 a.m. – 11:00 a.m.
Midmorning Break with Exhibitors
11:00 a.m. – 12:15 p.m.
Coding the comorbidities and conditions that impact pain management
Judi Blaszcyk
There’s more to managing chronic pain than treating the patient’s pain. Comorbidities can affect the level of E/M visits and determine which treatments a patient’s insurer will cover. During this session you’ll get the latest guidance on coding such conditions as:
-
Cancer
-
Hypertension
-
Diabetes
-
Injuries
-
Hardware
And because you can’t code it if it isn’t documented, you’ll get tips for educating staff about how to capture the information you need to support your diagnosis coding.
12:15 p.m. – 1:15 p.m.
Networking Lunch with Exhibitors
1:15 p.m. – 2:30 p.m.
“Experimental and investigational.” Now what?
Amy Turner
When a payer deems a covered treatment experimental or investigational it stops payments faster than you can say ‘Claim denied.’ In addition, practices need to know what to do when a provider wants to perform techniques such as mild® or iovera°. This session will show you how to:
-
Avoid the errors that will cause covered services to be flagged as experimental
-
Be aware and prepare for upcoming policy shifts
-
Implement the lessons learned in the Collections session to handle services the patient pays out of pocket
2:30 p.m. – 3:00 p.m.
Afternoon Break with Exhibitors
3:00 p.m. – 4:15 p.m.
Radiofrequency ablation – beyond the spine
Kayla Lee
You’re familiar with paravertebral facet joint denervation, now look beyond the spine to learn about the documentation and coding necessary to report denervation services used to treat such conditions as:
-
Chronic chest pain associated with shingles
-
Pudendal neuralgia
-
Morton’s neuroma
-
Osteoarthritis of the knee
4:15 p.m. – 5:30 p.m.
Drug billing – don’t compound mistakes that will cut your revenue
Amy Turner
It’s simple: A pain management practice that doesn’t accurately report the drugs it uses will lose money or receive overpayments that must be returned to the payer. To make matters worse, every recovery audit contractor recently began a complex review of drug claims to check for excessive or insufficient drug units billed. This session will show you how to streamline your drug billing process and eliminate errors with guidance on:
-
Keeping up with quarterly code and pricing updates
-
Accurate calculation and reporting units
-
Determining when and how to report waste
-
Reporting compounded drugs
MAIN CONFERENCE DAY 2
Wednesday, October 17
7:00 a.m. – 8:00 a.m.
Continental Breakfast with Exhibitors
8:00 a.m. – 9:15 a.m.
Head check: Document and report headache treatments
Judi Blaszcyk
It’s one of the most common types of pain. It can range from annoying to agonizing. And it has dozens of entries in the ICD-10-CM manual. It’s the headache and this session will show you how headaches and several common treatments for them should be documented, coded and reported.
9:15 a.m. – 10:30 a.m.
E/M in 2020 – unravel the proposed policies and new payment opportunities for 2020
Doris Branker
CMS has a lot of plans for E/M visits in 2020. The proposals to change documentation requirements and payments for office visits are capturing a lot of attention, but that’s just the start. In addition, CMS has plans to cut payment by 50% when a provider performs an E/M visit on the same day as a procedure. And there are new revenue opportunities as well: CMS intends to cover some non-face-to-face services such as interprofessional consults and new “virtual visits.” In addition, Interventional pain management doctors could have a new add-on code that would allow them to boost E/M revenue. Practices that aren’t ready if any of the proposals go into effect will lose money. Attend this session make sure your practice is prepared for anything CMS does.
10:30 a.m. – 11:00 a.m.
Morning Break with Exhibitors
11:00 a.m. – 12:15 p.m.
Nobody’s perfect – learn the mistakes made by the best coders and billers, and stop making them
Judi Blaszczyk, Doris Branker, Devona Slater, Stephanie Thomas
Our expert speakers see it all, as they help anesthesia and pain management practices around the country. They even see the mistakes made by billers and coders with years of experience. Come to this combined session to learn about the errors even experienced claims staff make and find out how to eliminate the mistakes from your practice.
12:15 p.m. – 12:45 p.m.
Ask the Experts – Open Q&A
12:45 p.m.
Conference Adjourns
HIERARCHICAL CONDITION CATEGORIES
MAIN CONFERENCE DAY 1
Tuesday, October 16
7:00 a.m. – 8:00 a.m.
Registration, Continental Breakfast with Exhibitors
8:00 a.m. – 9:00 a.m.
Keynote Presentation
The doctor is in: A clinician shares her top ICD-10-CM cures for common coding disorders
Erica E. Remer, MD, FACEP, CCDS, Founder and President, Erica Remer, MD, Inc. Consulting Services in Clinical Documentation, CDI, and ICD-10
Hierarchical conditions and quality-based revenue demand more accurate and complete diagnosis coding, supported by physician documentation. In this down-to-earth session, medical doctor and clinical documentation improvement expert Erica Remer, MD shares examples of commonly misunderstood ICD-10-CM guidelines and conditions. She’ll clear up your confusion and give you pointers to help your providers. Along the way, you’ll learn the most efficient ways to query physicians to get the full diagnostic picture of the patient’s condition and optimize your practice’s documentation, coding and reimbursement.
9:00 a.m. – 9:15 a.m.
Early Morning Break
9:15 a.m. – 10:30 a.m.
The ABCs of HCCs: All You Need to Know About Hierarchical Condition Categories Coding
Brenda Edwards
Risk adjustment coding under the Hierarchical Condition Category (HCC) model relies on accurate diagnosis coding to predict the cost of patient care. As Medicare Advantage plans proliferate and risk adjustment scores factor into CMS’ quality reporting programs, capturing precise diagnosis codes has never been more important. Learn how the HCC model steers your payment under certain insurance plans and how accurate documentation and coding makes a vast difference in revenue.
10:30 a.m. – 11:00 a.m.
Midmorning Break with Exhibitors
11:00 a.m. – 12:15 p.m.
2020 ICD-10-CM Update: Your Guide to Diagnosis Code Changes and Revisions
Brenda Edwards
Staying on top of the yearly revisions and updates to the ICD-10-CM code set is one of the best ways to maintain compliance with HCC coding and prepare for changes to code categories. Learn which families of diagnosis codes are expected to see changes in 2020 and get ahead of the new code updates that will impact your practice and your revenue stream.
12:15 p.m. – 1:15 p.m.
Networking Lunch with Exhibitors
1:15 p.m. – 2:30 p.m.
Take Heart and Take on Cardiology, Respiratory and Circulatory System Coding
Brenda Edwards
Take a deep dive into HCC coding and understand how to correctly report various heart ailments and respiratory issues. Highlights include atrial fibrillation, hypertension, COPD, cardio-respiratory failure and shock, lung cancer, angina, congestive heart failure, stroke and more.
2:30 p.m. – 3:00 p.m.
Afternoon Break with Exhibitors
3:00 p.m. – 4:15 p.m.
Avoid Hiccups: Stay Right with Gastro and Digestive System Coding
Brenda Edwards
Intestinal obstruction and inflammatory bowel disease are two of the conditions that fall under the digestive system portion of the HCC codes. Master your disease of the GI tract to accurately capture the full extent of your patients’ illnesses.
4:15 p.m. – 5:30 p.m.
Don’t Lose Your Nerve: Navigate Nervous System Coding
Brenda Edwards
From spinal cord injuries to paralysis and peripheral neuropathy, gain a comprehensive map of coding for nervous system disorders and clear up your confusion about difficult diagnoses.
MAIN CONFERENCE DAY 2
Wednesday, October 17
7:00 a.m. – 8:00 a.m.
Continental Breakfast with Exhibitors
8:00 a.m. – 9:15 a.m.
2020 HCC Outlook: Your Roadmap for Accurate HCC Coding in 2020
Brenda Edwards
Discover what’s in store for risk adjustment coding as the calendar flips to 2020 and be prepared to meet your diagnosis coding with authority in the new year. You’ll get a clear understanding of the changes to the HCC model so you can confidently report your claims and get paid for your services in 2020.
9:15 a.m. – 10:30 a.m.
Go More Than Skin Deep: Integumentary and Musculoskeletal System Coding
Brenda Edwards
When you treat conditions such as burns or chronic ulcers, as well as chronic conditions like osteoporosis, you’ll find a maze of possible diagnoses. Clear the confusion with a sound coding plan and draw the correct details from your documentation to meet the HCC score you deserve.
10:30 a.m. – 11:00 a.m.
Morning Break with Exhibitors
11:00 a.m. – 12:15 p.m.
Rev Your Engine: Master Endocrine and Metabolic Diseases Coding
Brenda Edwards
Coding for diabetes offers various nuances and details, from acute to chronic complications, that demand close attention to accurately convey your patients’ condition. Learn how to successfully report various stages of diabetes and an array of endocrine and metabolic diseases.
12:15 p.m. – 12:45 p.m.
Wrap Your Head Around Mental, Behavioral and Neurodevelopmental Disorders Coding
Brenda Edwards
Discover the vast array of behavioral and mental health conditions that fall under the HCC risk adjustment model, from major depression and paranoid disorders to schizophrenia and drug and alcohol dependence. Capture your mental health diagnoses with accuracy.
12:45 p.m.
Conference Adjourns
Exhibitor and Sponsorship Opportunities
Exhibitors at the Advanced Specialty Coding, Compliance, and Reimbursement Symposium get the exclusive opportunity to present to qualified decision makers looking for solutions to their practices’ICD-10-CM coding, compliance, billing, and reimbursement challenges.
Exhibitors will reach:
- Practice coders and supervisors
- Clinicians
- Coding educators and trainers
- Practice compliance managers
- Clinical documentation improvement specialists
- Practice managers and administrators
- Practice auditors and educators
- ASC coders
- Payer claims managers
- Nurses
- Physician assistants
Exhibitors
Healthpac
For information on exhibit and sponsorship opportunities, please contact
Carrie Dry
Approved for over 20 AAPC and AHIMA CEUs
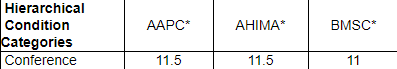
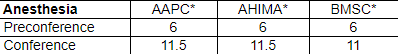
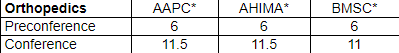
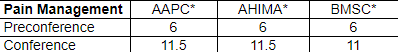

*CEUs are granted by the accrediting body (AAPC, AHIMA, BMSC)
Main Conferences:
This program has been approved for 11.5 continuing education unit(s) for use in fulfilling the continuing education requirements of the American Health Information Management Association (AHIMA). Granting prior approval from AHIMA does not constitute endorsement of the program content or its program sponsor.
This program has the prior approval of AAPC for 11.5 continuing education hours. Granting of prior approval in no way constitutes endorsement by AAPC of the program content or the program sponsor.
This program is preapproved by the Board of Medical Specialty Coding & Compliance (BMSC) for 11 CEUs towards the maintenance of the ACS, SCP and CCP-P credentials offered by BMSC.
Pre-Conferences:
This program has been approved for 6 continuing education unit(s) for use in fulfilling the continuing education requirements of the American Health Information Management Association (AHIMA). Granting prior approval from AHIMA does not constitute endorsement of the program content or its program sponsor.
This program has the prior approval of AAPC for 6 continuing education hours. Granting of prior approval in no way constitutes endorsement by AAPC of the program content or the program sponsor.
This program is preapproved by the Board of Medical Specialty Coding & Compliance (BMSC) for 6 CEUs towards the maintenance of the ACS, SCP and CCP-P credentials offered by BMSC.
Please contact the event manager Marilyn (marilyn.b.turner(at)nyeventslist.com ) below for:
- Multiple participant discounts
- Price quotations or visa invitation letters
- Payment by alternate channels (PayPal, check, Western Union, wire transfers etc)
- Event sponsorships
NO REFUNDS/TRANSFERS ALLOWED ON REGISTRATIONS
Prices may go up any time. Service fees included in pricing.
-----------------------------------------------------------------
This event is brought to you by:
BLR - NewYorkEventsList
http://www.NyEventsList.com
http://www.BostonEventsList.com
http://www.SFBayEventsList.com
-----------------------------------------------------------------
IVO180910CRE




